The Brain on Addiction: Understanding the Neuroscience of Addiction Test Results
March 10, 2026 | By Juliana Pace
The battle with addiction often feels like a constant fight against your own willpower. Many people ask themselves: "Why can't I just stop?" If you are struggling with a habit that feels out of control, you might feel guilty or ashamed. However, what if the real opponent is not your character, but specific changes happening inside your brain? Understanding the biological side of this struggle can change how you see your experience.
When you take an addiction test, you are measuring patterns in your behavior. These patterns are not random; they are driven by complex neurological shifts. Science shows that addiction is a chronic brain condition rather than a simple lack of discipline. This guide will help you understand the neuroscience of addiction in simple terms. By learning why your brain reacts the way it does, you can begin to find a clearer path toward change.
This article explores how substances and behaviors "hijack" the brain's natural systems. We will look at the chemicals that drive pleasure and the stress responses that make quitting so difficult. Most importantly, we will discuss how the brain can heal. If you have ever wondered about the science behind your habits, this exploration is for you.

How Addiction Tests Reveal Your Brain's Reward System
To understand the brain on addiction, we must first look at how the brain handles pleasure. Your brain is designed to reward you for survival behaviors, such as eating healthy food or spending time with loved ones. When you do something good for your survival, the brain releases a chemical signal that says, "That felt great, do it again."
In a healthy brain, this reward system is balanced. It helps you stay motivated and focused on your goals. However, addictive substances and certain behaviors change the way this system functions. They hit the "reward button" much harder than natural activities do. Over time, this intense stimulation rewires the pathways that govern your choices and priorities.
The Dopamine Connection: Pleasure, Reward, and Your Brain
Dopamine is often called the "feel-good" chemical, but its role is actually more about motivation and learning. It acts like a "save" button in your brain. When you experience something pleasurable, dopamine tells your brain to remember the cues that led to that feeling. This is why just seeing a specific place or person can trigger a strong urge to engage in a habit.
In the context of dopamine addiction, the brain is flooded with much higher levels of this chemical than it was ever meant to handle. Imagine a radio that is designed to play at a normal volume. Addiction is like turning that radio up to the maximum level for a long time. Eventually, the speakers begin to wear out. To protect itself from the noise, the brain reduces the number of dopamine receptors. This is why people often feel "numb" to everyday joys once an addiction takes hold. You can learn more about your own reward patterns by using an online assessment today.
From Experiment to Habit: The Neurological Pathway of Addiction
The transition from trying something new to having a deep-seated habit happens in a specific part of the brain called the basal ganglia. At first, a behavior might be a conscious choice managed by your prefrontal cortex—the part of the brain responsible for logic and planning. You decide to play a game or have a drink because it seems fun.
However, as the behavior is repeated and dopamine continues to flood the system, the "habit circuit" takes over. The brain begins to bypass the logical prefrontal cortex. The behavior becomes automatic, much like brushing your teeth or tying your shoes. This is why many people find themselves engaging in an addictive behavior before they even realize they have started. The neurological pathway has become a "superhighway," making it the path of least resistance for your brain.
The Brain's Stress Response: Why Anxiety and Cravings Intertwine
Addiction is not just about seeking pleasure; it is also about escaping pain. As the reward system becomes less sensitive, another part of the brain becomes hyperactive: the stress system. This shift explains why the "honeymoon phase" of a habit eventually turns into a cycle of anxiety and relief.
When the brain is used to a high level of stimulation, it views the absence of that stimulation as a threat. This creates a state of constant biological stress. For many, the drive to use a substance or engage in a behavior is no longer about feeling "high." Instead, it is about trying to feel "normal" or to quiet the intense signals of the brain's stress center.
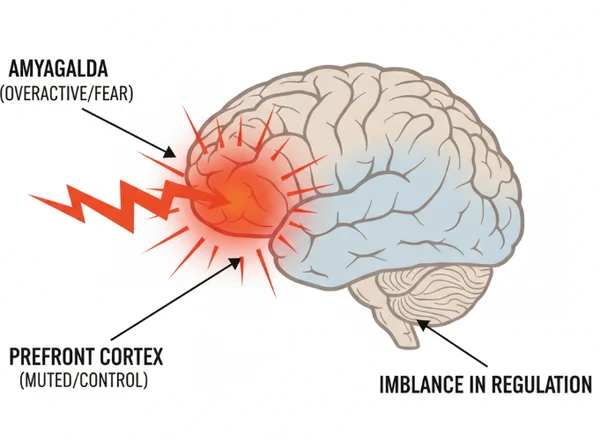
When Your Brain's "Off Switch" Stops Working: The Amygdala and Craving
The amygdala is a small, almond-shaped structure in the brain that handles emotions like fear and anxiety. In a brain struggling with addiction, the amygdala becomes oversensitive. It begins to treat the "craving" for a substance or behavior as a life-or-death emergency. This is why cravings can feel so physical and overwhelming.
At the same time, the prefrontal cortex—your "off switch"—becomes weakened. This part of the brain is supposed to say, "Stop, this isn't a good idea." But under the pressure of a hyperactive amygdala, the off switch fails to work correctly. The result is a powerful internal conflict. If you feel like your "off switch" is struggling, you can start the test to see where you stand and get more clarity on your situation.
Tolerance and Withdrawal: The Brain's Adaptation Mechanisms
The brain always seeks a state of balance called homeostasis. When you repeatedly introduce a substance or behavior that changes your brain chemistry, the brain adapts by pushing back in the opposite direction. If a substance makes you feel relaxed, the brain will respond by making you more alert and anxious to compensate.
This leads to two major issues:
- Tolerance: You need more of the substance or behavior to get the same effect because the brain has "turned down the volume" on its receptors.
- Withdrawal: When you stop the behavior, the brain's "push back" continues, leaving you in a state of physical or emotional pain.
These mechanisms are purely biological. They show that your body is trying to protect itself, even though the result makes you feel much worse. Understanding this can help remove the shame often associated with withdrawal symptoms.
Neuroplasticity: How Recovery Changes Your Brain
While the news about how addiction changes the brain can seem scary, there is a very hopeful side to neuroscience: neuroplasticity. This is the brain's incredible ability to change, grow, and repair itself throughout your life. Just as the brain can be rewired toward addiction, it can also be rewired toward health and balance.
Recovery is essentially the process of training your brain to build new pathways. It is like carving a new trail in a thick forest. At first, it is difficult and slow. But the more you walk the new path, the easier it becomes, and the old, addictive "superhighway" eventually begins to grow over and fade away.
Can the Brain Heal? Understanding Recovery Neuroplasticity
Yes, the brain can heal. Research shows that once a person stops the addictive behavior, the brain begins to restore its dopamine receptors and balance its stress levels. This process is called neuroplasticity recovery. It does not happen overnight, but the brain is remarkably resilient.
In the first few weeks of recovery, the brain is still in a state of imbalance. This is why early recovery is often the hardest part. However, over months and years, the prefrontal cortex regains its strength. The "logical" part of the brain learns how to manage the "emotional" signals from the amygdala again. Cognitive functions, memory, and emotional regulation can all see significant improvement as the brain stabilizes.
How Different Treatments Influence Brain Recovery
Different types of support work by targeting various parts of the brain's recovery process. For example:
- Cognitive Behavioral Therapy (CBT): This helps strengthen the prefrontal cortex by teaching it how to identify and "veto" the automatic thoughts coming from the habit circuits.
- Mindfulness and Meditation: These practices help calm the amygdala, reducing the intensity of the stress response and cravings.
- Healthy Habits: Regular exercise and good sleep provide natural, low-level dopamine hits that help the reward system reset.
Using a tool to get a personalized report can help you understand which areas of your life need the most focus. AI-driven insights can show you how your specific behaviors align with scientific scales, giving you a roadmap for your unique recovery journey.
Summary: Understanding the Brain Science Behind Your Test Results
The science behind addiction reveals important insights about your brain and behavior. It helps you realize that your struggles are not a sign of a "broken" personality. Instead, they are the result of a brain that has adapted to intense stimulation. When you view addiction through a scientific lens, the shame begins to lift, and practical solutions become visible.
The results of an assessment tool are more than just a score. They represent where your brain's reward and stress systems currently sit. Knowing your risk level is the first step in taking back control. Whether you are dealing with substances, internet use, or other behaviors, the principles of neuroscience remain the same: your brain can change, and you can lead the way.
As you consider your own relationship with addiction, remember that understanding your brain's responses is the first step toward meaningful change. Recovery is a journey of rewiring your mind for a richer, healthier life. If you are ready to see where you are on this journey, the best time to start is now.
Frequently Asked Questions About Addiction Neuroscience
Is addiction really a brain disease?
Yes, most major medical organizations, including the American Medical Association, define addiction as a chronic brain disease. This is because it causes clear, measurable changes in the brain's structure and function, specifically in areas related to reward, stress, and self-control. Understanding this helps people seek medical and psychological help without feeling like they have failed a moral test.
How does the brain change during addiction recovery?
During recovery, the brain undergoes a process of "re-normalization." Dopamine receptors that were shut down begin to reappear, allowing you to feel pleasure from normal activities again. The prefrontal cortex, which handles decision-making, becomes physically stronger and better at communicating with the rest of the brain. You can take an addiction test to start monitoring your own awareness and progress.
Can medication help restore the brain's balance?
In some cases, yes. Certain medications can help stabilize brain chemistry during the withdrawal phase or block the dopamine "spike" from substances. This can give the brain the "breathing room" it needs to begin the natural process of neuroplasticity. However, medication is usually most effective when combined with therapy and lifestyle changes.
What brain regions are most affected by addiction?
The three primary regions are the basal ganglia (the reward and habit center), the amygdala (the stress and emotion center), and the prefrontal cortex (the logic and impulse control center). Addiction typically strengthens the first two while weakening the third, creating a "perfect storm" that makes self-regulation difficult.
How long does it take for the brain to heal from addiction?
The timeline varies for everyone and depends on the type and duration of the addiction. Some chemical balances begin to reset within days or weeks. However, more significant structural changes—like the rebuilding of the prefrontal cortex—usually take several months to a year of consistent healthy behavior. The brain is always working toward healing as long as it is given the right environment.
Disclaimer: The information provided in this article is for educational purposes only and does not constitute medical advice or a formal diagnosis. While online screening tools can provide valuable insights, they are not a substitute for professional clinical evaluation. If you believe you are struggling with addiction, please consult a qualified healthcare provider or mental health professional.